Lessons Learned from 12 Days in The Hospital
Posted: January 4, 2019 Filed under: Uncategorized 3 Comments
I didn’t sleep a wink last night wondering how my Dad was doing in the ICU. I called his night nurse around 10 to check in and someone else answered and said he would call me back. By 11:15 when I hadn’t heard from him I called again. The not knowing was difficult. Dad was still sedated, but was doing well. The news of that still didn’t help me sleep so I was up very early and at the ICU by 7:00.
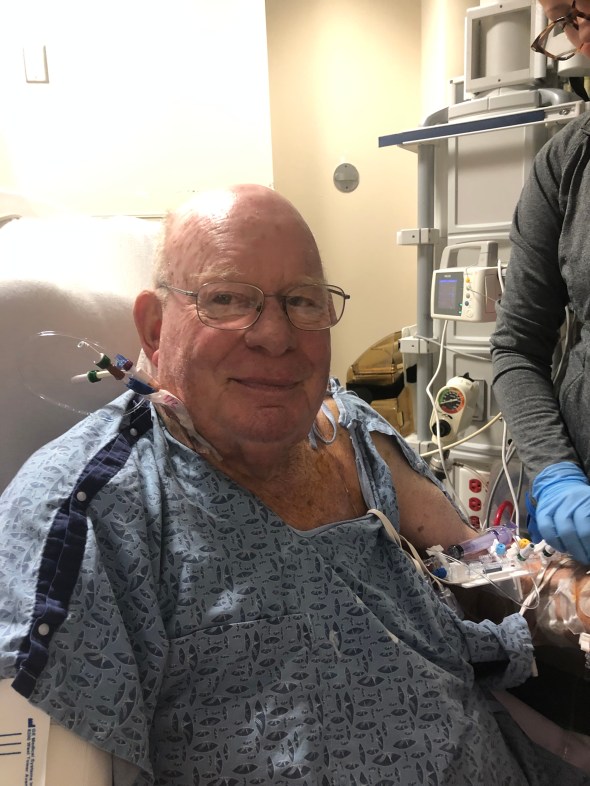
I walked into Dad sitting up in a chair still with many tubes and wires attached to him giving the OT and his ICU nurse more trouble than he should have. Here was the reason I didn’t sleep. I need to be there to smooth things over. I recognized that he had not eaten or drank anything in 36 hours. They brought him a breakfast tray and I gave him his coffee. What a difference his coffee makes. He became his most charming self.
I knew he was feeling much better based on the return of his rosy complexion. He bonded with his ICU nurse over favorite Bloody Mary recipes and all was good in the world. The good news came when two of his doctors came in and said he could leave the ICU and a bed in the step down unit was ready.
Once in his new and last hospital unit his great nurse today told him that if he met a couple of requirements he could go home tomorrow. That was music to his ears since we were told he could be there until maybe Monday or a Tuesday. The requirements were to walk and to pee before 5:00 PM.
My Dad has been an over achiever in everything about his heart so far. First he had an undetected heart attack where his body grew an new artery around the one that died from this heart attack some years back. Then when his heart valve failed he only had something like 8% capacity, yet he still lived on. So if you tell him he had to walk and pee you know he was going to do that.
His step down until was full of other people all needing to walk so the hallway like a slow nascar track. At first he did four laps with the Swedish walker. Then Carter brought lunch and my Mom came for a visit. You can see from the picture that everyone is back to regular life, all on their phones at the same time.

After lunch, Mom and Carter left and it was back to walking. Dad did six laps of the hall, lapping multiple other patients. We took another break for him to push fluids so the peeing could begin and then he walked three more laps. In total he did 2/3 of a mile. He tried to negotiate a later pee deadline with his nurse, but it turned out he didn’t need it. He passed all his tests.
His surgeon, Dr. Williams came in to see him. I was in the hall getting ready to leave. I told him of passing the tests and Dr. Williams looked in his window and said, we never have people ready to go this fast from this procedure. He went in and confirmed with my Dad that he was well enough to go and he said, “How about tomorrow morning?” You didn’t have to ask him twice.
So tomorrow morning will be my final trip to Duke to pick my Dad up and drive him back to the farm. It will be a big day. Sadly at the same time Carter needs to go to the airport to fly back to Boston. I have had a lot of quality time with my Dad, but no time with my Daughter. It was not the Christmas break we were looking forward to, but it was one where Carter got to keep her grandfather.
Lessons learned from this whole experience:
If you keep falling asleep in the middle of the day you might have Congestive Heart Failure.
If you start retaining a lot of fluids, you might have CHF.
If you have any hallucinations, you might have CHF.
If your breathing becomes labored, you got it…
Things that make your hospital stay more comfortable:
Bring your own toilet paper and Kleenex if you need it to be soft.
Your own pillow is very important. Hospital pillows are made for prisons.
A foam gel mattress pad is also a nice luxury if you value sleep’s restorative powers.
Negotiate with your doctor for the nurses not to disturb you between midnight and six in the morning.
Get real food from the outside world as long as it complies to your dietary restrictions, especially better coffee.
Bring head phones and a device to watch movies or listen to music.
Have a bossy family member to stay with you all the waking hours so they can advocate for you.
Bring your own things to sleep in that have pockets to hold your heart monitor.
Shave any part of your body that has any hair where they might put tape or sticky pads.
Follow orders, but don’t be afraid to ask for things.
Be nice to nurses and doctor!
Send you care giver on a nice vacation when you get better.
Thinking about you Ed…..we send love and prayers…..love all of our Wilton memories .. MY
love to you Janie….thanks Dana…..
Ed, know you will have a great recovery
And, yes, you are an over achiever!
I am sending my best from cape cod to
You, Janie and the family!
I will alway remember your fantastic Christmas Eve parties in Wilton for all generations! Those fabulous ham biscuits and superb southern hospitality!!!
Enjoy life to the fullest!!
Cheers!
1/4/2019
Peg shipman
We need to have lunch. Jack has had all of this. Especially the blocked artery and growing new things to take the place of that blocked artery. Unlike your Dad who was exercising by doing farm work etc. Jack was exercising at the center religiously. It saved his life. And I – like you have learned a lot about what to do in a hospital including your wonderful comment about the pillows. We take them even when we go,to the emergency room which we have unfortunately done a lot. Your Dad sounds a lot,like my Jack.
Carol Walker